Chronic stress chronically elevates cortisol, and chronically elevated cortisol directly suppresses testosterone production. Lowering cortisol through sleep, structured exercise, dietary changes, and evidence-backed supplements creates the hormonal environment in which testosterone can recover naturally. For most busy professionals, lifestyle changes drive 80 percent of the result. Supplements close the remaining gap.
The best testosterone booster in Pakistan is not always a pill. For busy professionals dealing with demanding workloads, disrupted sleep, and chronic stress, the relationship between cortisol and testosterone is the root issue, and no supplement addresses it effectively unless the lifestyle driving elevated cortisol is tackled first. This guide covers both sides: the natural strategies that work and where targeted supplementation fits into the picture.
For a broader overview of what is available, the testosterone booster supplements Pakistan guide covers the supplement landscape in detail. This article focuses on the foundational lifestyle strategies that make any supplementation more effective.
Table of Contents
The Cortisol-Testosterone Connection Every Busy Professional Needs to Understand
Cortisol and testosterone are produced from the same precursor: pregnenolone. When your body is under chronic stress, it prioritises cortisol production at the expense of testosterone synthesis. This is sometimes called the pregnenolone steal, and it is one of the most direct explanations for why stressed, sleep-deprived professionals so commonly experience the signs of low testosterone including low energy, reduced libido, poor gym performance, brain fog, and difficulty managing body weight.
The cascade works as follows. Chronic stress, whether from work pressure, financial anxiety, relationship strain, or poor sleep, keeps the HPA axis (hypothalamic-pituitary-adrenal axis) in a state of prolonged activation. The adrenal glands secrete cortisol to manage this sustained stress load. As pregnenolone
is diverted to cortisol production, the gonadal pathway that produces testosterone is starved of its raw material.
Understanding hormonal imbalance in men in this context reframes the problem entirely. For most busy professionals, low testosterone is not a primary condition. It is a secondary consequence of chronically dysregulated cortisol. This distinction is important because it determines the correct approach. Addressing cortisol first is not just preferable, it is the prerequisite for meaningful testosterone recovery.
Sleep Is the Most Powerful Cortisol and Testosterone Lever
No lifestyle intervention has a greater impact on both cortisol regulation and testosterone production than sleep, and it is the variable most consistently sacrificed by busy professionals.
Testosterone is synthesised primarily during deep sleep, with the majority of daily testosterone production occurring during the slow-wave and REM sleep stages. Research consistently shows that men who sleep fewer than six hours per night have significantly lower testosterone levels than those sleeping seven to nine hours. One study found that restricting sleep to five hours per night for one week reduced testosterone levels by 10 to 15 percent, an effect that would take months of pharmaceutical intervention to replicate in the other direction.
Cortisol follows a diurnal rhythm that peaks in the morning and gradually declines through the day, reaching its lowest point during sleep. When sleep is insufficient or fragmented, this rhythm is disrupted. Cortisol remains elevated in the evening when it should be falling, which further impairs the sleep stages during which testosterone is produced. The cycle is self-reinforcing: poor sleep elevates cortisol, elevated cortisol impairs sleep quality, and both suppress testosterone.
For busy professionals, protecting sleep is not a lifestyle luxury. It is a hormonal necessity. The practical priorities are consistent sleep and wake times even on weekends, blackout curtains and a cool room temperature, no screens for at least 30 minutes before sleep, and no caffeine after 2pm. These four changes alone move the needle more than any supplement.
Exercise Type and Volume Matter
Exercise is one of the most potent natural stimulators of testosterone, but the type, duration, and frequency matter significantly. Getting this wrong, particularly in the direction of overtraining, actively suppresses testosterone and elevates cortisol.
Resistance training with compound movements, squats, deadlifts, bench press, rows, and overhead press, produces the sharpest acute testosterone response of any exercise modality. Heavy multi-joint lifts involving large muscle groups signal the greatest hormonal adaptation. For busy professionals with limited time, two to four sessions of 45 to 60 minutes focusing on these compound patterns delivers superior hormonal benefit compared to six sessions of lighter, longer training.
Intensity matters more than volume for testosterone. Working in the four to eight repetition range with loads that challenge you produces a stronger hormonal response than moderate-weight, high-repetition training. The goal is to be done in under an hour. Training sessions exceeding 60 to 75 minutes begin to elevate cortisol acutely in ways that blunt the testosterone benefit of the session itself.
Excessive endurance training without adequate recovery also suppresses testosterone and elevates cortisol chronically. Long, daily cardio sessions are among the most common hormonal mistakes made by professionals who are trying to manage stress through exercise but inadvertently adding physiological stress on top of psychological stress. Two to three moderate cardio sessions per week alongside resistance training is a more hormonal-friendly balance. Boosting testosterone naturally through diet and exercise requires this kind of structured approach rather than simply doing more.
Diet and What You Eat Directly Shapes Your Hormonal Environment
Diet and hormonal balance are inseparable. Testosterone is a steroid hormone synthesised from cholesterol, which means dietary fat, specifically saturated and monounsaturated fat, is not the enemy of hormonal health. Diets very low in fat consistently correlate with lower testosterone levels in research studies. This is particularly relevant in Pakistan where fat-phobic dietary advice is common and where low-fat diets are sometimes adopted as part of weight management.
Adequate protein intake supports testosterone by providing the amino acid building blocks for hormonal precursors and by preventing muscle loss, which is a secondary driver of testosterone decline. Aim for 1.6 to 2g of protein per kilogram of bodyweight daily from whole food sources like eggs, meat, fish, dairy, and legumes.
Specific testosterone-boosting foods that are well supported by evidence and readily available in Pakistan include eggs, which provide cholesterol and vitamin D; fatty fish or fish oil for omega-3s; nuts especially almonds and walnuts for zinc and healthy fats; beef and liver for zinc and B vitamins; and pomegranate, which has shown measurable effects on testosterone in controlled trials.
Low testosterone and weight gain create a damaging feedback loop that diet directly addresses. Excess body fat, particularly visceral abdominal fat, contains aromatase enzymes that convert testosterone into oestrogen. Maintaining a healthy body composition through dietary discipline is one of the most effective long-term strategies for preserving testosterone levels as a professional ages.
Alcohol deserves specific mention in the context of the Pakistani professional lifestyle. Even moderate regular alcohol consumption suppresses testosterone by impairing Leydig cell function in the testes and elevating cortisol. Reducing or eliminating alcohol is one of the highest-leverage dietary changes available.
Stress Management and Practical Tools for Professionals
Lowering cortisol requires active management of the psychological and physiological stress load, not just hoping the workload eases. For busy professionals, the most practical and evidence-supported approaches are as follows.
Breathing and meditation practices have a direct and measurable impact on cortisol levels. A practice as brief as ten minutes of slow, diaphragmatic breathing or guided meditation activates the parasympathetic nervous system, suppresses sympathetic activation, and reduces salivary cortisol within a single session. Research on consistent meditation practice shows meaningful reductions in baseline cortisol over weeks to months. For professionals who dismiss meditation as impractical, physiological sighing, which involves a double inhale through the nose followed by a long exhale through the mouth repeated five times, achieves a similar acute cortisol-lowering effect in under two minutes.
Time-blocking and boundaries around work hours directly reduce the chronic HPA axis activation that drives cortisol dysregulation. The absence of psychological recovery periods during and after the workday is a structural problem that no supplement addresses. Protecting two to three short recovery blocks during the day, even five to ten minutes of non-screen downtime, maintains cortisol within a more functional range than continuous cognitive loading without breaks.
Social connection and laughter have measurable cortisol-lowering effects that are undervalued in a professional context. Regular quality time with family, friends, or colleagues outside of work tasks supports the hormonal environment more than most people realise.

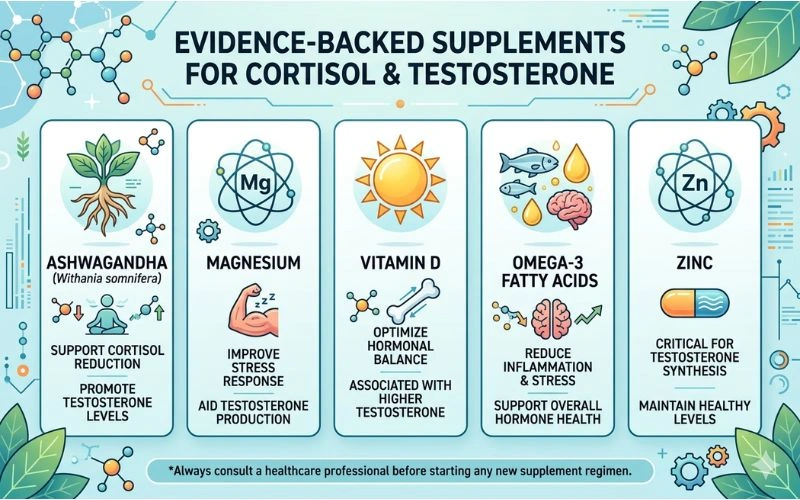
Evidence-Backed Supplements for Cortisol and Testosterone
Once lifestyle foundations are in place, targeted supplements can meaningfully accelerate hormonal recovery. The evidence here is considerably stronger for some compounds than others, and the natural testosterone boosters that work are a shorter list than supplement marketing suggests.
Ashwagandha
Ashwagandha is the most consistently evidence-supported adaptogen for both cortisol reduction and testosterone elevation. Multiple randomised controlled trials show that 300 to 600mg of KSM-66 or Sensoril standardised ashwagandha root extract reduces morning cortisol by 14 to 32 percent compared to placebo, with corresponding improvements in testosterone, sperm quality, and self-reported stress over eight to twelve weeks. Adaptogens for stress management like ashwagandha work precisely because they modulate the HPA axis rather than simply stimulating alertness the way caffeine does. For Pakistani professionals, an ashwagandha supplement standardised for withanolide content is the most practical starting point among all adaptogenic options.
Magnesium
Magnesium is the most widely deficient mineral in high-stress populations and one of the most impactful for both sleep quality and testosterone. Stress depletes magnesium rapidly through urinary excretion, and most Pakistanis do not consume adequate magnesium through diet. Low magnesium is directly associated with higher cortisol and lower testosterone. Supplementing with magnesium glycinate, the most bioavailable and gut-friendly form, at 200 to 400mg taken before bed improves sleep depth, reduces cortisol, and supports testosterone production through multiple pathways. It is also one of the most cost-effective supplements available.</p></p>
Vitamin D
The Vitamin D functions as a steroid hormone precursor and plays a direct role in testicular testosterone synthesis. Vitamin D receptors are present on Leydig cells, and deficiency is directly correlated with lower testosterone. Given that Pakistan has extremely high rates of vitamin D deficiency despite abundant sun exposure, supplementing with 2,000 to 4,000 IU of D3 daily is a high-priority foundational step for most Pakistani professionals. Get your serum 25(OH)D tested if possible and aim for a level between 50 and 80 ng/mL.
Omega-3 Fatty Acids
Omega-3 for hormonal health operates through multiple mechanisms. EPA and DHA reduce systemic inflammation, which is a cortisol driver. They also support the cellular membrane composition of Leydig cells, improving their capacity for testosterone synthesis. Research shows that men supplementing with omega-3s have measurably higher testosterone and lower cortisol than matched controls. A daily dose of 2 to 3g of combined EPA and DHA from a verified fish oil is a practical and well-tolerated addition to any hormonal recovery stack.
Zinc
Zinc is a rate-limiting mineral for testosterone synthesis. The enzyme that converts cholesterol to pregnenolone, the starting point of testosterone production, is zinc-dependent. Exercise increases zinc loss through sweat, and stress elevates urinary zinc excretion. Pakistani diets are frequently low in bioavailable zinc, particularly for those who consume primarily plant-based foods. Supplementing with 25 to 45mg of zinc per day, ideally as zinc picolinate or zinc bisglycinate, supports both testosterone and the immune functions that chronic stress compromises.
When to Consider Professional Support
Understanding TRT vs natural support is important context for any professional exploring this space. Testosterone replacement therapy is a medical intervention appropriate for men with clinically confirmed hypogonadism, where testosterone levels are significantly below normal range despite consistent lifestyle optimisation. It is not a shortcut for healthy men whose levels are low-normal due to lifestyle factors.
For most busy professionals in Pakistan, a full blood panel including total testosterone, free testosterone, SHBG, LH, FSH, cortisol, vitamin D, zinc, and thyroid function provides a complete hormonal picture. This baseline, taken in the morning before eating, tells you exactly where the deficiencies and imbalances lie and allows you to target supplementation precisely rather than guessing.
If after three to six months of consistent sleep, structured training, dietary discipline, stress management, and evidence-backed supplementation your testosterone remains clinically low, that is the point at which a conversation with an endocrinologist about medical options becomes appropriate.
Building a Daily Routine That Supports Both Goals
The most effective approach is not a collection of isolated interventions but a coherent morning routine and daily structure that supports cortisol regulation and testosterone production simultaneously.
A practical framework for busy professionals looks like this. Wake at a consistent time and get morning sunlight exposure within 30 minutes, which sets the circadian rhythm and supports both cortisol’s natural morning peak and vitamin D synthesis. Eat a protein and fat-rich breakfast that includes eggs, nuts, or meat rather than a high-carbohydrate breakfast that elevates insulin and blunts the morning testosterone window. Take your vitamin D, zinc, and omega-3 with this meal. Train in the late morning or early afternoon where possible, since testosterone naturally peaks in the morning. Keep sessions under 60 minutes and compound-movement focused. Take your ashwagandha and magnesium in the evening. Protect your sleep window non-negotiably.
This framework does not require additional hours in the day. It requires reorganising existing hours around hormonal priorities rather than around convention and convenience.
Frequently Asked Questions
How long does it take for cortisol to normalise after making lifestyle changes?
Acute cortisol changes from better sleep and stress management are measurable within days. Baseline cortisol levels typically normalise over four to twelve weeks of consistent lifestyle changes. Ashwagandha supplementation accelerates this process, with significant cortisol reduction measurable at six to eight weeks in clinical trials.
Can a busy professional realistically implement all of these changes at once?
Not all at once, and trying to do so adds stress rather than reducing it. The priority order is sleep first, then dietary protein and fat adequacy, then structured resistance training twice per week, then supplementation. Add one element at a time over four to six weeks rather than overhauling everything simultaneously.
Will these natural approaches work as well as testosterone replacement therapy?
For men with lifestyle-driven low testosterone, natural approaches often restore testosterone to healthy levels without the side effects or costs of TRT. For men with primary hypogonadism, the natural approaches will not fully compensate and TRT becomes appropriate. The critical distinction is whether low testosterone is secondary to lifestyle factors or primary to a medical condition. A blood panel with a doctor’s interpretation answers this definitively.
Is there a specific time of day to take ashwagandha for cortisol reduction?
Evening dosing of ashwagandha is generally preferred because it works with the natural cortisol decline that occurs through the afternoon and evening. Taking it 30 to 60 minutes before bed also supports the improved sleep quality that is consistently reported in ashwagandha trials. Morning dosing is a secondary option if evening dosing causes any mild digestive sensitivity.
Which single change has the greatest impact on testosterone for a busy professional?
Sleep, without a close second. Consistently sleeping seven to nine hours per night at regular times has a more powerful effect on testosterone than any supplement, dietary change, or exercise modification. Every other intervention in this article works better when sleep is adequate and works poorly when it is not.